News
-

-

-

Fauquier Health CEO Receives National Recognition
June 20, 2025Rebecca Segal, FACHE receives national recognition
Learn more -

-
Fauquier Health Publishes 2024 Community Benefit Report
May 19, 2025Report outlines hospital’s continued impact on the health and economic vitality of Fauquier County
Learn more -

-
Fauquier Health Earns Top Honors from Lifepoint Health
March 11, 2025Hospital and CEO celebrated for outstanding quality and operations performance in 2024
Learn more -

Fauquier Health Names DAISY Award Honoree
February 12, 2025PACU nurse receives honor after two previous nominations
Learn more -

-

Fauquier Health Earns 2024 Leapfrog Top Hospital Award for Outstanding Quality and Safety
December 18, 2024We are one of only 36 hospitals nationwide and the only one in Virginia to be named a Top General Hospital.
Learn more -

Fauquier Health Earns an ‘A’ Hospital Safety Grade from The Leapfrog Group
November 15, 2024For the second time this year, Fauquier Health has received national recognition
Learn more -

Fauquier Health Names DAISY Award Honoree
November 04, 2024Interventional Radiology Nurse Receives Recognition for Second Time
Learn more -

Fauquier Health Cardiac Rehab Program Earns Certification
October 22, 2024Program receives repeat honors
Learn more -

Fauquier Health Names DAISY Award Honoree
September 05, 2024Family Birthing Center Nurse recognized as extraordinary
Learn more -
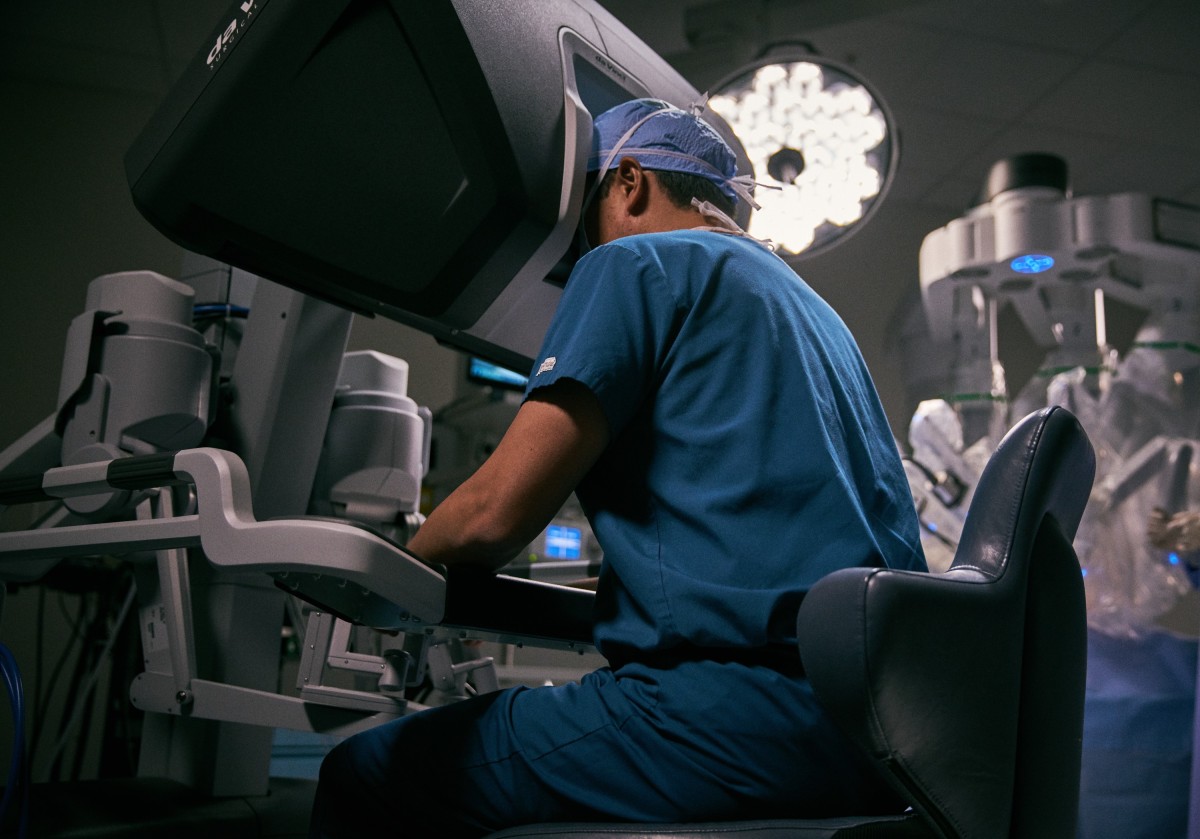
Fauquier Health Community Day
August 09, 2024Test your surgical skills on the Da Vinci Robot, participate in interactive demonstrations and go on "behind the scenes" tours at this FREE community event!
Learn more -

Back to School is a Great Time to Head Back to the Doctor
July 24, 2024Start healthy habits early; make regular check-ups part of your child's routine says Dr. Ghuman.
Learn more -

Don't Ignore Abdominal Pain
June 04, 2024A hernia is one of the most common reasons for surgery in the United States. Left untreated, it can become a medical emergency.
Learn more -

Fauquier Health Names Mercy Award Honoree
May 28, 2024Patricia Jeffries nominated by fellow staff members.
Learn more -

Fauquier Health Names DAISY Award Honoree
May 14, 2024ICU Nurse recognized as extraordinary
Learn more

